“Have great hopes and dare to go all out for them. Have great dreams and dare to live them. Have tremendous expectations and believe in them.”
~ Norman Vincent Peale
The Nuclear Option
As we made our way through November, the effects of the chemo were being experienced as they unfolded, presenting themselves with each infusion in real time. While I had reams of documents and pamphlets telling me what to expect, I only understood once the side effects started to manifest themselves throughout my body and my mind. My only focus was to get through each treatment as quickly and effectively as possible; to me, nothing else mattered at this point…or did it? My treatments were every 2 weeks and I was injected with nuclear medicine and steroids from Monday to Wednesday. Then for the next week and a half, I would swim upstream to get to the good days as soon as possible. Initially it took until the first weekend after the Monday treatment, before I would begin to feel better.
One thing Steph did struggle to find online were stories of survivors and families that experienced pancreatic cancer and the challenges they experienced during treatment. As you heard in part 1, she found a lot of information on the severity of my cancer, but she also discovered that there was a dearth of experiences out there to help us get through the process: some sort of virtual, ‘What to expect while they kill the tumor inside my body’. The mental gymnastics we had experienced with this cancer to this point has been exhausting on so many levels. We began to dig to find some sort of self-help. I have come to rely on Google and YouTube over the last few years to help resolve most issues that I encounter. Whether it’s fixing a toilet, a pool pump, raising kids, whatever, chances are someone has put some media out there that I’ve used to get me out of a jam. Having said that, on more than one occasion, I have found myself stuck with a disconnected toilet, a disassembled appliance, an extra part or even angrier teenagers, with nothing to help me get to the next step, except figuring it out myself. I am putting my story out here, not because I think I have all the answers, or that anyone cares (although the outpouring of support has been incredibly heart-filling). I am putting it out here because, this maze of physical and mental challenges can wreak havoc with many of the lives connected to a journey through illness and recovery. If I can help get one person through a day with a small amount of insight or understanding, to achieve even a small shred of success while battling any disease, it will be worth it.
I was definitely overconfident after my first treatment and I thought I would get through this without a struggle. But, every session would remove one or two good days off the total fourteen days between treatments. My taste buds would mostly recover by about the Wednesday of week two, but the neuropathy hung around a lot longer…yes, lovely neuropathies; they immediately presented themselves as a result of chemo. I could not eat or drink anything cold – even water. If I tried, the stinging and burning, like glass shards, overcame my mouth and throat; cold water, soda, ice cream, were suddenly out of my life. My fingertips and feet were also extremely sensitive to cold…more stinging, like pins and needles. The first bite of anything caused the muscles in my jaw and throat to contract painfully for a very long 10 seconds and my body felt as if it was constantly buzzing during the infusion period. These effects lingered for as long as they wanted to, without any real pattern adherence except that it was taking longer to recover after each session. In fact, it wasn’t until a month after my last chemo did most of this dissipate. Some of it returned when I started radiation, but I’ll save that for later.
November turned into December: month one, done. My dad had to get back to Toronto to manage his own prostate cancer treatment. Mom stayed to help until mid-December so she had taken over the cooking and spent the rest of the time fretting over me. I hoped she was also enjoying the beautiful fall weather we were having in AZ compared to Toronto. It was the longest she had ever been away from my father and all this while he was going through his own battle with cancer. She was a blessing and key to getting me through the first phase. My oncologist had given me two main directives: don’t lose weight and don’t get sick (cold, flu, infection). Either or both could interrupt my chemo schedule or corrupt the actual therapy, so my focus was on eating and staying healthy. Mama’s cooking can’t be beat and that was exactly what I needed.
As part of my bi-weekly, nuclear liquid loading, I was also filled with anti-nausea and anti-diarrhea drugs that I believe worked. I didn’t vomit once and the other thing, well I got lucky there too. However, I was constantly nauseous; head spinning, mouth-watering, pit of your stomach sick, with meat-sweats and all. Regardless, I was not going to lose weight. If you know me, you know I really enjoy a good meal so I knew I could make that work and mom really helped. Chemo also does quite a number on your white blood cells and your general immunity so, homemade chicken soup, staying home or wearing a mask whenever I left the house were mandatory. In fact, I can honestly say that I had been in some form of lockdown since November: pre-COVID-19. I was focused on those two directives and as part of this workstream, we were not going to lose any time because of weight loss or illness.
Crazy house
To say we had a lot going on in the house was an understatement. Anything and everything were testing our allegiance to our goal of being as normal as possible and while the intention was to maintain a regular rhythm, we were struggling to make it happen. The guilt was starting to weigh me down. I had separated my mom from my dad, and I didn’t feel we were really appreciating her efforts in the moment. I couldn’t be there for my wife and my kids while I was passed out on the couch. Lucidity and wellness were becoming more difficult with each passing day and my family witnessed all of it because I was occupying couches everywhere. I could have gone to my room when I couldn’t deal, but I could not imagine what spending hours or days in bed would have done to my psyche. I needed to be around everyone whether I was conscious or not. The steroids were turning me into a real asshole. I was mouthy and irritable most of the time. I didn’t mean to be, and unfortunately no one was safe from my glare or occasional biting words. That was difficult and surreal; it was as if I was standing outside of myself, hearing what I was saying and just as the words left my mouth, I wanted so badly to reel them back in…not good. During this time, I could tell the very instant that the good days had arrived – I felt totally different. It was like a weight had been lifted off of me; I was so relieved when that switch finally flipped. On those good days, I crammed in whatever I could…small mundane tasks like taking out the garbage and straightening stuff up to wanting to go to the grocery store, leave on a road trip or take a hike. These weren’t always possible, but it was a good day if I felt that ambitious.
I wasn’t paying attention to how this was really affecting my family. I just expected everyone was taking it all in stride. Life outside of my abdomen was expected to carry on and proceed with no discernable impact to our everyday lives. That was the mandate; follow the plan and get the goal. Well, that isn’t how this works. I wasn’t thinking about how this was affecting Steph. She was dealing with the stress of her dad’s illness while juggling work pressures; so much time spent coordinating her schedule, her dad’s schedule along with my appointments, all while dealing with my crabby, sick ass. Every aspect of our life had now been turned upside down and too many specific plans needed to be shelved. Uncertainty crept into every detail of our days. What would this do to us financially? Did we have enough health insurance? What about wills and medical directives? Life insurance? The week I went to my doctor for the first time, we were supposed to be travelling to Toronto: our first out of country vacation in a while, an opportunity to see my family, especially my dad – cancelled. Steph hadn’t been feeling 100 percent healthy before all of this: how was this affecting her now? Being groggy, irritable, nauseous and full of radioactive chemicals a good percentage of the time, makes communication and everything else difficult, even with family. Everything was disrupted; the natural ebb and flow of the house had been disturbed and it didn’t matter that we were getting help, it was all different. Releasing control to everyone else is not something I have ever found easy and even Steph was starting to struggle. Add to all of this, the coming holidays and needless to say, there was a significant amount of stress hanging over all of us.
Ben was diagnosed with a tumor on his kidney at about the same time they found out what was going on with me. His kidney was removed in November, and while he championed through the surgery, now being permanently on dialysis, he was beginning to physically struggle with the process and the changes in his life. He kept thinking he would get back to normal, but this dream was fading fast for him. His health was up and down, but mostly down. I tried to do what I could with doctor’s appointments and just trying to be supportive, but I had started to become useless to both Ben and Steph. The chemo sessions had been wearing me out more and more and good days were getting shorter every session. I remember attending an appointment with Ben as he visited his cardiologist. After tending to him and serving up his usually diatribe on the evils of salt, the doctor began making some notes, and then turned his direction to me, ‘what’s with the mask?’, he was kind of a gruff guy. ‘I’m going through chemo, I have pancreatic cancer’, I responded as cold and matter-of-factly as the question was posed, his posture sagged. ‘Hmm, that’s too bad’ he responded and went back to his notes. Ben and I looked at each other and I could see him shake his head. I realized that no matter what he was going through, he was worried about me and he didn’t want whatever he was going through to interfere with my treatment. Ben was a tough guy with a heart of gold…more on him later.
Where’s the Wisdom?
My son was in his first few months of high school. At 14, what was he really going through as he watched all this unfold in such a heavy environment? I took talking for granted and assumed my fighting attitude was ringing a positive vibe. I assumed that he understood that the effects of the chemo were deleterious, and it wasn’t really me. I never asked or checked in with him as I was too caught up in dealing with my physical and mental limitations. He was witnessing the physical deterioration of both me and his grandfather. Two close male role models in his life were struggling hard. He is not as gregarious as the girls so even though we did have family talks, he wasn’t getting a lot of airtime. The girls were trying to maintain their cadence of work, school and social needs, and the changing rythmn was surely affecting them. My girls began to spend a lot more time at the house and with my parents also in town, it was getting a little crowded. Work hours were being piled on too, as the holidays were getting closer. Alex was getting ready to graduate and Allie and Olivia were dealing with their finals and end of year assignment wrap ups. All that exciting and stressful energy as they prepared: exams, certifications, ceremonies, parties, grad pictures, and other preparations. Yet they made time to be with me during some infusions. They were present at more meals. Every couch and room was full. I had become a mere observer of what was unfolding in my own home: a passive participant, distracted by my own morbidity. Looking back, I think there is so much more I should have been saying, asking, and I should have been listening more closely.
Needless to say, when this much pressure builds up within any vessel, the inability to release or resolve some of that pressure inevitably leads to an involuntary release of that pressure. I wish I could tell you it was all singing and dancing, hugging and laughing, roses and sunshine at my house…but that’s not my family. Every once in a while, a little yelling, crying, reckoning and resolving was necessary; so, we did. We came to expect that things were going to blow up once in a while, but we also knew it would be better once we regrouped and slowed things down a little.
How could I let the pressure build up like that? Why didn’t I notice it and address it sooner? I am supposed to be the elder in this house. When you’re faced with your own mortality you may believe that, all of the sudden, you will be filled with the wisdom and courage to sort it all out and keep it together for yourself and those that surround you. You may believe that significant adversity will instantly provide you with all of the right things to say to calmly manage any situation. Challenges will provide you with the perfect story or anecdote to assuage any doubts and fears, and most importantly, provide you with a viable solution to solve any problem…well, not me. My mortality had me lost for some time. I had no idea and my focus was firmly fixed on getting through the first phase of treatment. It wasn’t until I started to force myself to be more reflective, that I realized how much I couldn’t see. One thing that became important and even necessary to cope with just about anything, was my own ‘elasticity’. How much could I bend before I broke and how much could I listen before I spoke. Problems didn’t present themselves when I lost my way…the problems happen when I don’t stop soon enough to ask for directions and recalibrate my path. Now, I am not saying I have figured it all out. I just hope that, I have learned that sooner rather than later, when I find myself lost, I stop to ask for directions and get back on the right path…hopefully.
‘Roid Rage
I’ll be the first to admit, I’m not the easiest person to live with; I have been known to be critical, combative, obsessive, a little over-bearing and sometimes a pain in the ass. Put me on steroids and make me sick most of the time, well I was becoming a whole new kind of special. My focus had to change. I was not my disease or the drugs that were trying to save me. It wasn’t until December and January that I had decided, any optional medication had to stop.
Side note: after my very first chemo session, somewhere there is a picture of my father and I, at the bottom of my drained pool, finishing the clean-up – I had my portable infusion machine strapped on and a mop in my hand. It was a fair description of the Panacci way: adversity is squashed by hard work – that didn’t last too long, but it felt great while it lasted.
I had to manage my symptoms from the chemo with more meditation and prayer instead of medication. I began to spend more hours on the couch or in the backyard, staring at a square patch of fabric or the roses until the nausea went away. I became proficient at breathing through whatever was washing over me. I would wake up and immediately turn to reading to distract me from my own irritability. I do love the fact that I have read so much more than usual during this time. I had pulled out books that I hadn’t read in a while, added a few new ones and focused on a couple of poets to get me through. I’ll include my chemo reading list at some point. It was hard not to go back to the Lorazepam, Ondansetron, Montelukast, Prochlorperazine, Loperamide, Dexamethasone, Oxycodone or whatever else I was taking. I couldn’t deal with the negativity they brought along with their relief.
I need this to be clear: I am not saying that everyone would have the same reaction as I had to these medications, but I do know what they did to me. I will not say that I overcame nausea and the weight loss that comes with the other two symptoms without the help of pharmaceuticals, but the reactions I was having, began to become more detrimental than helpful, so I tried alternatives. When nausea and neuropathy became really unbearable, and breathing or reading weren’t working, I turned to more herbal remedies that helped. Even though those had their own side effects, they were much easier to handle than the pharmaceuticals…and they made me laugh…a lot.
December
Despite everything that was going on, I believed early on in December there was an undercurrent of optimism in our home. There was a plan that was being executed and we were following it as best as we could. Strangely, I even enjoyed putting up the Christmas lights for the first time in years. Now, I did them on a good day and made sure I took no medication before I went up the ladder. It was the first time I had put up lights without the help of a few beers. My dad made his way back to Scottsdale for a while, friends were coming over and helping us with meals and just spending some time laughing and being together. Allie and Olivia were busy working and going to school, Aidan was wrapping up his first semester and Christmas was coming. I was so proud of all my kids. However, the event of the month was Alex’s was graduation. Years of hard work were about to pay off for her and she would have a job offer lined up before she even graduated. We celebrated by attending her pinning and graduation ceremonies at GCU and then having a party at our place. We planned it so that it took place during my good days and it really was a good night with everyone who attended. I was exhausted, but my spirits were lifted. I love a good party and the energy it brings, even without alcohol. It felt so good to be around my family and friends in this setting. I needed a good time and that was a wonderful event to celebrate.
I was eating and trying to stay healthy when, I got too cocky. I needed to get a flu shot and couldn’t avoid it any longer. I had planned to venture out of the house – I felt great and it had been a while since I was out alone. I am definitely an extrovert most of the time, but I do like to be alone once in a while and that had not been available to me for several weeks. Don’t get me wrong, I love having people around, especially my family, but I needed some space too. Before stopping at the Walgreen’s for my shot, I made a stop at the post office inside the Ace Hardware near our home…as I write this, I have no idea why. It was close to Christmas, so the line was a little long, but I had time. As I waited, I began to notice how close people get to each other in a line, it was the Seinfeld episode that hadn’t been written – ‘Close Standers’. In ‘a second’, my knees began to throb, and that pain started to creep up into my pelvis, as if someone just punched me in the lower abdomen…then the dizziness kicked in and I was not feeling very good at all. I was next in line and was trying to ignore whatever was happening. As I left the store, thunder clapped, and the rain began to fall as I made my way to the car, but not without getting wet. The drive home was slow because of the rain and thank goodness, the dizziness was getting worse. I pulled into the garage and went straight for the couch with a blanket; just breathe, I thought. Steph checked my temperature and we called the Mayo triage line. I was hitting 100 degrees and that meant a trip to the ER…ugh. They swabbed my sinus, filled me full of fluids, shot me up with Tamiflu and sent me on my way a few hours later. No mask, a compromised immune system and an overconfident patient – that would have been my comment for the file if I was the attending nurse.
The Holidays
The rest of the month was much better. All the gifts I needed to purchase came from Amazon since I was not taking a chance anywhere out in public. Opening presents and a huge breakfast filled Christmas morning, then, as if on some unspoken queue, everyone flopped on the couches watching Netflix, eating and relaxing…this continued until about midnight, when we finally decided to pack it in. It was a beautiful day. Movies, documentaries, cookies and Steph’s home-made chicken enchiladas…delightful. I cannot remember holding the kids’ attention for that long during any Christmas Day and it truly was magical. The Family Stone, The Two Popes, The Lunch Box Gang, a movie about Judy Garland and so many more. There was no rhyme or reason to what was being watched, we were just together and that’s what mattered. It was the most relaxed Christmas Day ever.
New Year’s Eve came and went at an even slower pace. The kids were all doing their own thing and Ben joined Steph and me. He was staying over, and it was no surprise when we both passed out on the couch well before 10:00 PM…Steph was stuck in the middle trying to be festive, I think. I can’t really remember. I had an infusion session on December 30th so I wasn’t dancing on tables and I hadn’t had a drink since early October. I was a lump on the couch and not even the start of a new decade was going to change that, unfortunately. But 2020 was here and the general consensus was that more than a few of us were ready for 2019 to be over…right.
2020: Send it back
The political environment, and the rumors of a possible virus out of China may have been all over the news, but they were not front of mind during those first couple of weeks of January. Ben was struggling with his dialysis and we were urging him to come live with us; we would get him lined up with a dialysis unit down here in Scottsdale instead of him having to go to Prescott. We were not impressed with the level of care he was receiving (remember his cardiologist) so we figured things had to change…we just needed to work out logistics. Aside from New Year’s Eve and Day, he wanted to be at home, despite our urgings. He was getting weaker and we knew he wasn’t watching his diet. Earlier in 2019, Steph had booked a few days away for the family during the second week of January, at the new Great Wolf Lodge that had opened in Scottsdale. It was unlikely that I would go because of the risks, so we decided that the kids should still attend and have some fun. Even though they were older, a few days out of the house and in a happy environment would be a great thing. Check-in was scheduled for the 9th of January, and I was going to have the results of my latest CT scan on the 8th. We anticipated that we could be celebrating and the positive thoughts were focused on praying for a shrinking tumor.
On January 7th, while in the throes of discomfort from my last infusion, I felt it again; the creeping soreness and fever had come back. My joints ached and I didn’t know what the hell was going on…well, I did. I was getting sick again and I was worried that it would screw up the schedule for my scan the next day. I was pissed and scared and watched as my temperature hovered around 99 degrees. I was not going anywhere if it didn’t hit 100…then it hit 100 and Steph brought me back to the emergency room. The lobby was packed with people coughing, sniffling, even vomiting into blue bags provided by the nurses. As one nurse took my blood pressure and temperature, she apologized for the fact that they were jammed – a super busy flu season was keeping them constantly busy. The good thing about being immunocompromised is that they don’t leave you in the emergency room waiting area too long. Within an hour they determined that I picked up another virus, but they couldn’t tell what it was, even after another brain scratching nose swab. Fluids were pumped into me and I waited. The attending doctor had assured me that this shouldn’t affect my scans the next day as it wasn’t as severe as it felt. Relief: the last thing I wanted was any delay of either those scans, future infusions, anything. I lay on the emergency room table and I believe it was about 8 PM when my phone rang: it was Ben.
At first, he sounded somewhat normal for how he was lately, but I could tell something more was wrong. He kept saying he wasn’t feeling well and then came out with the fact he wrecked the truck on his way home from dialysis. After more probing, he told me he had jumped a curb, but it was dark and he couldn’t tell if the truck had been damaged. He was able to drive home but he just wasn’t feeling very well. We sent Allie to pick him up and get him back to our place. He was not in good shape, and the report from Allie about his house convinced us he was not going back up there until we got him balanced and back to some sort of normal. He was staying whether he wanted to or not.
Good news…
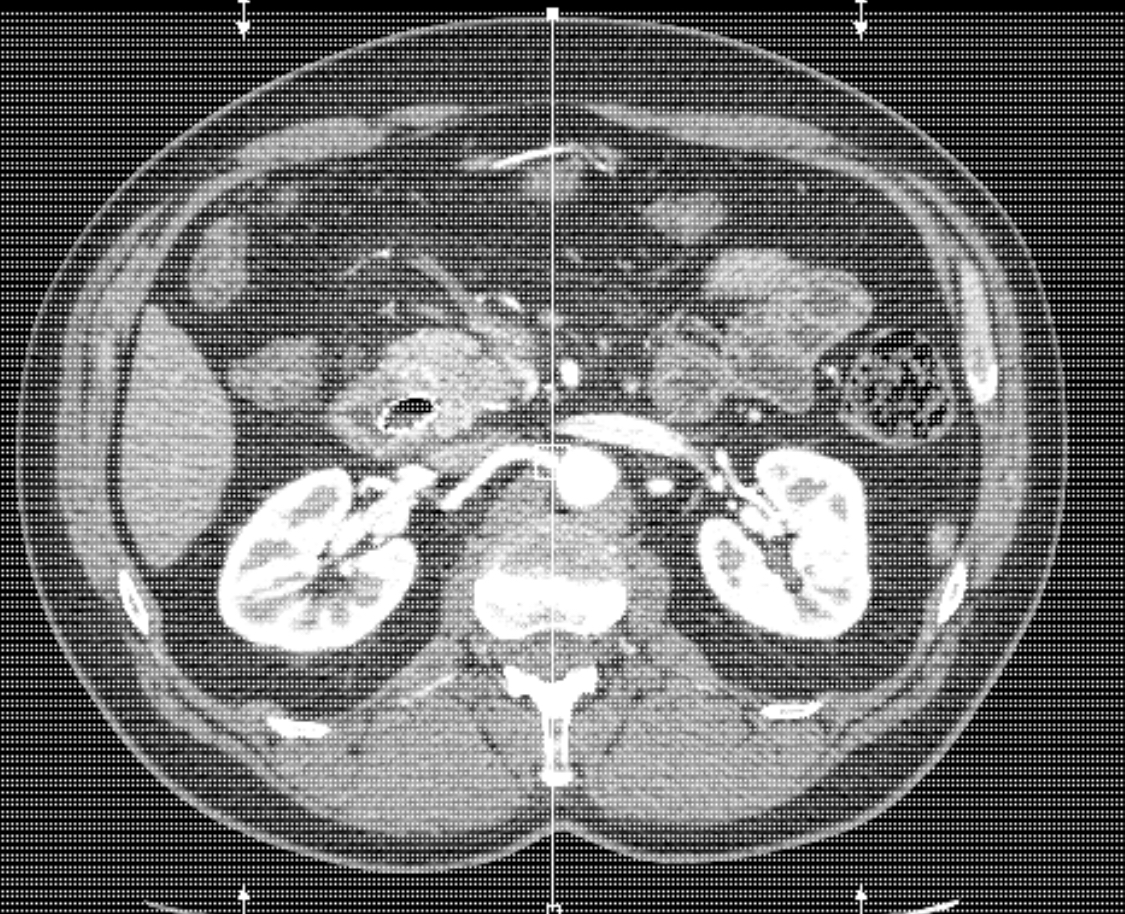
It was January 8th, I made it to my scans at the other Mayo campus in east Scottsdale. They were CT scans with contrast so that means, as you are being imaged, they fill you with fluid that light up any areas of concern – they literally glow. This will have been the third time I have gone through this process and it is frankly one of the weirdest procedures I had ever experienced. The actual imaging is not a problem. You lay on the table, shirt off, pants down to your knees and hold your breath as you go back and forth through a big donut shaped x-ray machine. The weird part is the contrast. Once they release it into your veins, the familiar metallic taste of heparin and saline fills your mouth and throat. Then, it feels as if gallons of warm liquid fill you up inside, like a wave from your neck to your pelvis…surreal, gross, and just strange. The first time I had this done, the technician described it as ‘feeling like you wet yourself’…really? Regardless, I was excited to be done and couldn’t wait to get the results. Mayo is absolutely great about getting results out the same day. Usually, they are posted in the patient portal, but the scans required my oncologist to explain them so we made our way to his office. He came in smiling as usual, sat down and without hesitation, said “you’ve done very well” like I had just passed a history test. He explained that the tumor had shrunk to 1.7 cm from the 3.5 cm originally scanned when this all started – HALF!! It shrunk by half!Whatever I was going through physically and emotionally, it was all worth it to hear him say, ‘it shrunk by almost half!’ I was literally on cloud nine and Steph just looked shocked. He explained that we would stay the course with a few more infusions, then we would plan for radiation. As he left, Steph broke down in tears of joy, releasing a lot of pent up tension waiting for this moment. I had no doubt it was working. The poison they were injecting me with and the way it was making me feel, had to have some upside…it was working. We couldn’t get home fast enough to tell the kids: good news from the doctor, then a few days away for them to celebrate this milestone. There were shouts and tears and lots of happiness when we got home. We decided we were going to celebrate with cake! Allie went to the store for at least two bakery cakes and ice cream. The celebration was short lived.
Ben was here and although he too was smiling from the news, he was visibly weak. We all sat in the family room until everyone had gone to either prepare dinner or pick up cake. He and I tried to talk but we were both worn out. The contrast always has some dragging effect on me. I usually feel more tired and nauseous and today, that was on top of being in the middle of my last chemo treatment. He and I had no energy, but it seemed comforting just to sit together, slumped on the couch. I remember thinking, we needed to get him back to his doctor or any doctor as soon as possible tomorrow. “Dinner’s ready” was eventually shouted from the kitchen. Both of us slowly worked our way up from the clutches of the couches, but as he rounded the corner, I could see Ben’s legs give out and he slowly sank to the ground. Everyone rushed to his side and gently helped him into the other room; he was annoyed with the fall and all the fussing, but he seemed ok. He had hardly a bite of dinner but did manage a couple of bites of cake before making his way back to the couch. Steph and Alex agreed they had to get him to the hospital. The hours leading up to the morning were rough. Ben coughed incessantly, and in between bouts, argued with Steph throughout the night and early hours of the morning that he was not ready to go to the hospital. I heard some of the conflict from my bed upstairs, but I couldn’t move. Morning finally came and Steph was not going to listen to his fight to avoid the hospital; he had to go. The kids helped get him into the car and Steph had taken him to be checked out. The kids then began to prepare for their check in to the lodge.
Heartbreaking
The next 48 hours quickly became another mega loop on this fucking emotional roller coaster. My mind was a blur, so the facts I am relating are from the detailed notes Steph kept. I could never relate in words, the emotions that were experienced during this time. Every blood pressure test, bacterial tests, everything had been captured. Ben’s blood pressure at admission, 89 over 32 (normal is 80) and his breathing and coughing were becoming even worse, if that was even possible. Doctors thought he was anemic and needed a blood transfusion. They were admitting him immediately and taking blood cultures to check for bacterial infection. Steph stayed with him most of the day and night while Ben urged her to go home and be with me. He was getting more confused about what was going as doctors and nurses worked on him with great urgency. Looking back at it all, we often wonder if he didn’t have one of the early cases of COVID-19. Steph said his cough was gut wrenching and blood, along with some orange substance was presenting itself in his sputum. As day turned to night, Ben continued to urge Steph to go home. It was later in the evening when she asked him if he would be ok if she left, he nodded approvingly for her to go. Their last words to each other: Steph said “I love you” and squeezed his big toe. “Love you too kid” he responded. She left the hospital.
I woke up in the middle of the night hearing Steph on the phone with the doctor: it was just after 1 AM. He was letting her know that Ben had agreed to go on a ventilator, and he was currently on life support in a chemically induced coma. The coughing and hacking would not subside and that was their only option. Tests showed he may have a significant blood infection and could go into septic shock. His blood pressure was so low, they had him on maximum pressers (medication) to keep it beating. They said he needed time to rest, but when Steph asked how long he would be intubated and on life support, there was an inaudible response on the other end of the phone, then everything went silent. ‘At least two days, maybe seven, if he wakes up’…If? ‘His body is very sick’ the doctor responded.
January 10th: as the sun was rising, I was accompanying Steph to the hospital; I was gloved and masked up for safety. The kids were at the Lodge and we had picked up Steph’s sister Kelly to take her to see their father. I vividly remember walking into the ICU room, Ben was unrecognizable, and I knew right then, he was not going to get better. He was heavily sedated, and the doctors were struggling to explain what the hell was going on…a virus was attacking his blood, his oxygen and his heart. In turn, his body was trying to protect his organs so his extremities were suffering. His hands and feet were turning gray as his blood focused on protecting his heart and lungs. I stayed for as long as I could, but then had to leave. At 11:39 AM Ben’s heart monitor alarm began to chime louder as he hit 178 BPM…Steph shouts, “holy shit” and stands up, thinking his heart was going to explode. A flood of nurses and doctors are begin appearing on both sides of the door as Steph holds his hand and watches his heart rate monitor. Ben’s brother Bill, niece Jennifer, daughter Kelly and her boyfriend Kyle surround him as Ben’s breaths begin to get longer and deeper. I remembered it was close to noon when Steph had called. “Please pick up the kids and bring them to the hospital; they’ll be waiting for you at the front of the lodge. Without hesitation I got in the car and made my way to the kids. As we hurried to the hospital, the attending nurse confirms with Steph that he was passing…time of death 11:57 AM.
The doctors confirmed Ben had enterococcus pneumonia which caused him to go into septic shock and further strained his already weakened heart. At that very moment, everyone’s heart cracked.
The next few weeks were charged with emotions at the highest level. My oncologist agreed to some extra time off chemo so I could participate with funeral needs and attend the ceremony in a somewhat lucid and participative state. Steph went into extreme task mode: a process I had watched her sink into when her grandmother passed. Her focus turned to getting things done. She began to organize the ceremony, contact Ben’s coworkers, friends, and family. She began organizing pictures for the memorial, sorting his bills, searching funeral homes, contacting the cemetery and whatever other affairs needed to be handled. I knew it was her way; whether to avoid grief temporarily or simply ensure she honored her father by being collected and responsible. Steph had already lost her mother at a young age, now she was orphaned, and I knew the pain inside her was screaming to get out. Nothing could have prepared anyone, especially Steph for the incredible void left by Ben. She was devasted and her grief, deep and painful…it still is today.
There is so much to say about Ben. He was definitely someone you were glad to know. He could strike up a friendship and conversation with anyone and he welcomed me into his life without hesitation.
The funeral was a beautiful service attended by so many of his friends and family, many who had travelled to come pay their respects. Cousin Jennifer had arranged to have the reception at her home. Steph’s uncles from her mother’s side helped with the catering and the celebration of Ben’s life was a comforting event as everyone gathered to remember Ben with food, drink and surrounded by familial companionship. However, once the funeral is over, and the celebration of life wraps up, loved ones are left with their own thoughts and memories, along with the ‘what ifs’ and the ‘whys?’. There are times when your heart is so broken, you can never be convinced the wound will heal. Neither time, nor activity will can suppress the sadness and as each day passes, you swear the wound is only growing deeper…we thought life for our family had changed significantly up to that point…we had no idea; the impact of Ben’s death reverberated throughout every fiber of our family and we would deal with the compounding pain and stress over the coming months.
Thank you for taking the time to share this journey. I am sharing it in parts because so much has happened over the past 9 months (I rushed this one so please pardon the grammatical errors you might find). I have a few months more to share but as I release this, I am preparing for surgery. My plan is to deliver the rest of the story as soon as I can…from the very beginning of this unwanted journey, I have believed that not only could I survive this, but that I had to because I wasn’t ready to accept any other alternative. It has been a blessing to be in the care of the great doctors, nurses and support staff of the Mayo Clinic in Phoenix as well as to be surround by the loving and patient support of my family and the encouragement from all of you…thank you, and we’ll write to you soon. God bless.


Rob and Steph, what you have had to endure is beyond words. My thoughts and prayers are with you all. If there is anything I can do to help, please reach out. Sending hugs to you both.
LikeLiked by 1 person
Thank you Joyce 🙏
LikeLike